Achieving Health Equity: 2026 Policy Frameworks for a 20% Disparity Reduction

Achieving Health Equity: 2026 Policy Frameworks for a 20% Disparity Reduction
The pursuit of health equity is one of the most pressing challenges of our time. Despite significant advancements in medical science and technology, vast disparities in health outcomes persist across different populations, often along lines of socioeconomic status, race, ethnicity, geography, and other social determinants. These disparities are not merely statistics; they represent lives cut short, preventable illnesses, and untapped human potential. Recognizing the urgency of this issue, policymakers and public health advocates are increasingly focused on developing robust frameworks to address these systemic inequalities. This article delves into the ambitious goal of achieving a 20% reduction in health disparities by 2026, examining the innovative Health Equity Policies 2026 that are being proposed and implemented to turn this vision into a reality.
The journey towards health equity is complex, requiring a multi-faceted approach that transcends traditional healthcare delivery. It demands a deep understanding of the social, economic, and environmental factors that shape health, and a commitment to dismantling the barriers that prevent certain groups from achieving their full health potential. The 2026 target of a 20% reduction in disparities is not just a number; it represents a tangible commitment to creating a more just and equitable society where everyone has the opportunity to thrive. This ambitious goal underscores a shift from merely acknowledging disparities to actively intervening with strategic, evidence-based policies.
In the following sections, we will explore the core tenets of these emerging Health Equity Policies 2026, analyze their potential impact, and discuss the challenges and opportunities that lie ahead. We will also highlight the importance of collaboration across various sectors, from government agencies and healthcare providers to community organizations and individuals, in driving this transformative change. The conversation around health equity is evolving, and the focus on actionable policy frameworks for 2026 signifies a pivotal moment in this ongoing endeavor.
Understanding the Imperative: Why a 20% Reduction by 2026?
The decision to target a 20% reduction in health disparities by 2026 is rooted in both ethical considerations and practical realities. Ethically, it reflects a fundamental belief that health is a human right and that no one should be disadvantaged in their health outcomes due to circumstances beyond their control. Practically, persistent health disparities lead to significant economic burdens, including increased healthcare costs, lost productivity, and a diminished quality of life for affected communities. Addressing these disparities is not just about fairness; it’s about building stronger, more resilient societies.
The year 2026 provides a near-term, yet sufficiently challenging, horizon for measurable progress. Setting such a concrete goal helps to galvanize action, focus resources, and create accountability across different stakeholders. It encourages a shift from incremental improvements to more transformative interventions. The 20% target, while ambitious, is seen as achievable with concerted effort and strategic policy implementation. It serves as a benchmark against which the effectiveness of new Health Equity Policies 2026 can be rigorously evaluated.
Furthermore, the COVID-19 pandemic starkly illuminated and exacerbated existing health disparities, particularly among marginalized communities. This global health crisis served as a powerful catalyst, underscoring the urgent need for systemic changes in how health and social services are structured and delivered. The pandemic highlighted how factors like housing, employment, access to technology, and systemic racism profoundly impact health outcomes. Consequently, there’s a renewed political will and public awareness to tackle these issues head-on, making the 2026 target not just an aspiration, but a critical response to recent global events.
Defining Health Disparities and Their Drivers
Before delving into specific policies, it’s crucial to define what constitutes a health disparity. Health disparities are preventable differences in the burden of disease, injury, violence, or opportunities to achieve optimal health that are experienced by socially disadvantaged populations. These differences are often linked to social, economic, or environmental disadvantage and are not randomly distributed. Instead, they systematically affect groups who have historically experienced greater obstacles to health based on their racial or ethnic group, religion, socioeconomic status, gender, age, mental health, cognitive, sensory, or physical disability, sexual orientation or gender identity, geographic location, or other characteristics historically linked to discrimination or exclusion.
The drivers of health disparities are multifaceted and interconnected. They include:
- Socioeconomic Status: Income, education, and occupation profoundly influence access to resources, healthy environments, and quality healthcare.
- Environmental Factors: Exposure to pollution, lack of green spaces, and inadequate housing can lead to chronic health conditions.
- Healthcare Access and Quality: Barriers to accessing affordable, high-quality healthcare services, including insurance status, geographical location, and provider availability.
- Systemic Discrimination: Racism, sexism, and other forms of discrimination can lead to chronic stress, limited opportunities, and biased treatment within healthcare systems.
- Behavioral Factors: While individual choices play a role, these are often shaped by the social and economic contexts in which people live.
- Structural Inequities: Policies and practices embedded in social and economic structures that perpetuate disadvantage for certain groups.
Understanding these drivers is foundational to developing effective Health Equity Policies 2026 that address the root causes of disparities rather than just their symptoms.
Pillar One: Strengthening Social Determinants of Health (SDOH) Interventions
A cornerstone of the Health Equity Policies 2026 is a robust focus on the social determinants of health (SDOH). It is widely acknowledged that clinical care accounts for only a fraction of overall health outcomes, with factors like housing, food security, education, and economic stability playing a far more significant role. The new policy frameworks aim to integrate SDOH considerations more deeply into healthcare and public health planning.
Key Policy Initiatives under SDOH:
- Housing as Health: Policies promoting affordable, stable, and safe housing are crucial. This includes initiatives for rental assistance, combating housing discrimination, and investing in community development projects that improve housing quality. For instance, programs that connect individuals experiencing homelessness with housing and supportive services have shown significant improvements in health outcomes and reductions in emergency room visits.
- Food Security and Nutrition: Addressing food deserts and promoting access to nutritious, affordable food is paramount. This involves expanding SNAP benefits, supporting local food initiatives, establishing farmers’ markets in underserved areas, and integrating nutrition counseling into primary care. The aim is to ensure that healthy eating is an accessible choice for all, not a luxury.
- Education and Economic Opportunity: Investing in early childhood education, improving school systems in disadvantaged areas, and providing job training and employment support are vital. These policies recognize that educational attainment and stable employment are powerful predictors of long-term health. Programs that link individuals to living-wage jobs and offer financial literacy training can break cycles of poverty and improve health.
- Transportation Access: Ensuring reliable and affordable transportation to healthcare appointments, grocery stores, and job centers is critical. Policies may include expanding public transit, subsidizing ride-sharing for medical appointments, and investing in infrastructure that supports walking and biking.
- Community Safety and Green Spaces: Policies that reduce violence, improve neighborhood safety, and create accessible green spaces contribute significantly to mental and physical well-being. This includes community-based violence prevention programs and urban planning that prioritizes parks and recreational facilities.
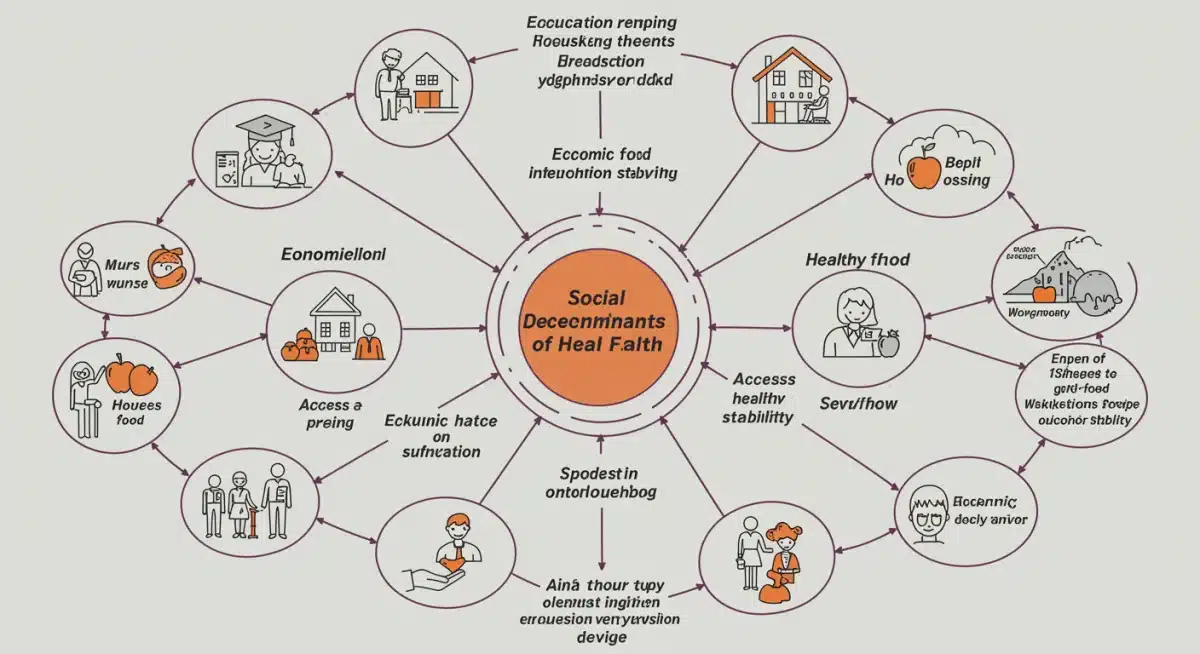
The integration of SDOH into healthcare systems is also a significant trend. This involves screening patients for social needs during clinical encounters and connecting them with appropriate community resources. This ‘upstream’ approach to health aims to prevent illness by addressing the root causes of poor health, rather than solely treating its symptoms. The Health Equity Policies 2026 envision a healthcare system that is not only reactive but proactively engaged in improving the social conditions that shape health.
Pillar Two: Enhancing Healthcare Access and Quality for Underserved Populations
While SDOH interventions address foundational issues, improving direct healthcare access and quality remains a critical component of Health Equity Policies 2026. This pillar focuses on dismantling systemic barriers within the healthcare system itself.
Key Policy Initiatives under Healthcare Access and Quality:
- Expanding Health Insurance Coverage: Universal or near-universal health insurance coverage is a fundamental step. Policies may include expanding Medicaid eligibility, strengthening marketplace subsidies, and exploring public health insurance options to ensure that financial barriers to care are minimized.
- Workforce Diversity and Cultural Competency: Addressing the lack of diversity among healthcare professionals is crucial. Policies aim to increase the representation of underrepresented groups in medicine, nursing, and allied health fields through scholarships, mentorship programs, and pipeline initiatives. Furthermore, mandatory cultural competency training for all healthcare providers is being emphasized to ensure respectful and effective care for diverse populations.
- Telehealth and Digital Health Equity: Leveraging technology to bridge geographical gaps in care is a priority. Policies promote the expansion of telehealth services, including broadband infrastructure development in rural and underserved areas, and programs to provide digital literacy training and devices to patients who lack them. This ensures that technological advancements reduce, rather than exacerbate, disparities.
- Community Health Centers and Primary Care: Strengthening the network of community health centers (CHCs) is vital. CHCs often serve as a lifeline for underserved communities, providing integrated medical, dental, behavioral health, and pharmacy services. Policies will focus on increased funding, workforce support, and expanding their capacity to reach more individuals.
- Data Collection and Disaggregation: To effectively measure and address disparities, granular data is essential. Policies advocate for improved data collection on race, ethnicity, language, socioeconomic status, and other demographic factors, and for the disaggregation of this data to identify specific areas of need and evaluate policy effectiveness.
The emphasis on these policies reflects a recognition that a fragmented and inequitable healthcare system cannot adequately serve a diverse population. By focusing on both access and the quality of care, particularly for those who have historically faced barriers, the Health Equity Policies 2026 aim to create a healthcare landscape that is truly patient-centered and responsive to the needs of all individuals.
Pillar Three: Addressing Systemic Racism and Discrimination in Health
Perhaps the most challenging, yet essential, pillar of the Health Equity Policies 2026 is the direct confrontation of systemic racism and other forms of discrimination within health and social systems. Decades of research have demonstrated the profound and pervasive impact of discrimination on health outcomes, both directly through biased treatment and indirectly through its influence on SDOH.
Key Policy Initiatives against Systemic Discrimination:
- Anti-Racism Training and Education: Implementing mandatory anti-racism training for all public sector employees, including healthcare providers, educators, and social workers. This training aims to raise awareness of implicit biases and structural racism, providing tools to counter discriminatory practices.
- Equity Audits and Impact Assessments: Requiring all new policies, programs, and budget allocations to undergo an ‘equity audit’ or ‘racial impact assessment’ to proactively identify and mitigate potential disparate impacts on marginalized communities. This ensures that equity is considered at the design stage, not just as an afterthought.
- Community-Led Participatory Approaches: Empowering communities most affected by health disparities to lead in the design, implementation, and evaluation of health policies and programs. This ensures that interventions are culturally relevant, effective, and truly responsive to community needs. Policies will support funding and infrastructure for community-based organizations.
- Fair Lending and Economic Justice: Policies aimed at combating discriminatory practices in lending, housing, and employment that disproportionately affect minority communities. This includes strengthening fair housing laws and promoting equitable investment in historically marginalized neighborhoods.
- Reforming the Justice System: Recognizing the link between the justice system and health outcomes, policies will advocate for criminal justice reform, including alternatives to incarceration, reducing recidivism, and addressing the health needs of incarcerated and formerly incarcerated individuals.
Addressing systemic racism requires a sustained, multi-generational effort. The Health Equity Policies 2026 are designed to initiate and accelerate this process by embedding anti-racist principles into institutional practices and public policy. It’s about moving beyond simply acknowledging the problem to actively dismantling the structures that perpetuate it.
Measuring Progress: Metrics and Accountability for 2026
Achieving a 20% reduction in health disparities by 2026 necessitates robust measurement and accountability mechanisms. Without clear metrics and transparent reporting, it will be impossible to assess the effectiveness of the implemented Health Equity Policies 2026 and make necessary adjustments.
Key Measurement and Accountability Strategies:
- Baseline Data Establishment: Before any intervention, establishing clear baseline data for various health disparity indicators is crucial. This includes metrics related to chronic disease prevalence, infant mortality rates, life expectancy, access to preventive care, and mental health outcomes, disaggregated by relevant demographic factors.
- Standardized Reporting: Developing standardized reporting frameworks across all relevant agencies and organizations to ensure consistent data collection and comparability. This will allow for aggregation of data and identification of national and regional trends.
- Public Health Dashboards: Creating publicly accessible health equity dashboards that track progress towards the 20% reduction goal. These dashboards can provide real-time data, highlight areas of success, and pinpoint areas needing more attention. Transparency is key to building trust and fostering collective action.
- Regular Policy Evaluation: Implementing a system for regular, independent evaluation of the implemented policies. This includes impact assessments, cost-effectiveness analyses, and qualitative research to understand the lived experiences of communities affected by the policies.
- Accountability Frameworks: Establishing clear accountability frameworks for government agencies, healthcare systems, and other stakeholders. This may involve setting specific targets for different entities and linking funding or performance incentives to progress on health equity metrics.
The success of the Health Equity Policies 2026 hinges not just on their implementation, but on the ability to demonstrate tangible results. A commitment to data-driven decision-making and transparent accountability will be paramount in sustaining momentum and ensuring that resources are directed where they can have the greatest impact.
Challenges and Opportunities on the Path to 2026
While the vision for a 20% reduction in health disparities by 2026 is inspiring, the path forward is not without its challenges. However, these challenges also present significant opportunities for innovation and collaboration.
Challenges:
- Political Will and Sustained Funding: Maintaining political commitment and securing adequate, sustained funding for long-term initiatives can be difficult, especially amidst competing priorities.
- Inter-sectoral Collaboration: Health equity requires collaboration across traditionally siloed sectors (health, education, housing, transportation, etc.). Building effective partnerships and coordinating efforts can be complex.
- Data Gaps and Quality: Despite calls for improved data, significant gaps in disaggregated data still exist, making it challenging to accurately assess disparities and the impact of interventions.
- Resistance to Change: Systemic changes can face resistance from entrenched interests or those comfortable with the status quo.
- Measuring Long-Term Impact: Some SDOH interventions may take years to show their full health impact, making it challenging to demonstrate immediate returns on investment within a short timeframe.
Opportunities:
- Increased Public Awareness: Growing public awareness and demand for social justice create a fertile ground for implementing bold health equity policies.
- Technological Advancements: Innovations in data analytics, telehealth, and digital health tools offer powerful new ways to reach underserved populations and monitor progress.
- Cross-Sectoral Partnerships: The necessity of collaboration can foster innovative partnerships between government, non-profits, academia, and the private sector, leading to more holistic solutions.
- Economic Benefits: Investing in health equity is not just a social good; it has significant economic benefits, including reduced healthcare costs and increased productivity, providing a strong economic argument for these policies.
- Learning from Global Best Practices: Opportunities exist to learn from and adapt successful health equity initiatives implemented in other countries and regions.
Navigating these challenges and leveraging these opportunities will be crucial for the successful implementation of the Health Equity Policies 2026. It requires agile leadership, adaptive strategies, and a steadfast commitment to the underlying principles of justice and fairness.
The Role of Community Engagement and Advocacy
No policy framework, however well-designed, can succeed without the active involvement and advocacy of the communities it aims to serve. Community engagement is not merely a formality; it is a fundamental principle of effective health equity work. The Health Equity Policies 2026 emphasize participatory approaches, recognizing that those closest to the problems are often closest to the solutions.
Community organizations, grassroots movements, and advocacy groups play a vital role in:
- Identifying Needs: Providing invaluable insights into the specific health challenges and social needs of their populations.
- Shaping Policies: Ensuring that policies are culturally appropriate, relevant, and address the unique circumstances of diverse groups.
- Facilitating Implementation: Serving as trusted intermediaries between formal institutions and community members, helping to disseminate information and facilitate access to services.
- Holding Systems Accountable: Acting as watchdogs, monitoring progress, and advocating for continued attention and resources for health equity initiatives.
Empowering communities through funding, capacity building, and genuine partnership will be a hallmark of successful Health Equity Policies 2026. This means moving beyond tokenistic engagement to true co-creation and shared decision-making, ensuring that the voices of marginalized communities are not just heard, but are central to the policy-making process.
Conclusion: A Future of Greater Health Equity by 2026 and Beyond
The ambitious goal of reducing health disparities by 20% by 2026 represents a critical turning point in the ongoing quest for health equity. The proposed Health Equity Policies 2026, spanning interventions in social determinants of health, improved healthcare access and quality, and direct action against systemic discrimination, offer a comprehensive roadmap for achieving this vision. This is not a simple task, but an undertaking that demands sustained political will, innovative collaboration, robust data-driven accountability, and profound community engagement.
The impact of achieving this 20% reduction would be transformative. It would mean fewer preventable illnesses, longer and healthier lives for millions, reduced economic burdens, and a more cohesive and just society. It would demonstrate that with focused effort and a commitment to address the root causes of inequality, significant progress is not only possible but imperative. As we look towards 2026, the success of these policies will depend on our collective ability to move beyond rhetoric and implement tangible, equitable solutions that benefit everyone.
The journey to full health equity is a long one, extending far beyond 2026. However, by setting and striving for this significant milestone, we establish a powerful precedent and build the foundational structures necessary for a future where health is truly a right for all, not a privilege for a few. The next few years will be crucial in demonstrating what is possible when societies commit wholeheartedly to the principle of health equity.





