Optimize Telehealth Workflows: Reduce Healthcare Costs by 10% in 2026

The landscape of healthcare in the United States is continuously evolving, driven by technological advancements, shifting patient expectations, and the persistent need for operational efficiency. In this dynamic environment, telehealth has emerged not just as a temporary solution during crises but as a fundamental pillar of modern healthcare delivery. For US healthcare systems, the imperative to reduce operational costs while simultaneously enhancing patient care is paramount. This article serves as a comprehensive guide, outlining how healthcare providers can strategically optimize telehealth workflows to achieve an ambitious yet attainable 10% reduction in operational costs by the year 2026. This target is not merely an aspiration; it is a strategic necessity that can be realized through thoughtful planning, technological integration, and a patient-centric approach to care delivery.
The Unfolding Promise of Telehealth in Cost Reduction
Telehealth, broadly defined, encompasses a range of technologies and services that deliver healthcare at a distance. Its adoption soared during the recent global health crisis, demonstrating its immense potential. Beyond its role in ensuring continuity of care during lockdowns, telehealth has proven to be a powerful tool for telehealth cost reduction. By minimizing the need for physical infrastructure, reducing administrative overhead, and improving resource utilization, telehealth offers a clear pathway to significant financial savings.
Understanding the Current Cost Landscape in US Healthcare
Before delving into optimization strategies, it’s crucial to understand the major cost drivers in US healthcare. These typically include:
- Administrative Overheads: Complex billing, scheduling, and record-keeping processes.
- Infrastructure Costs: Maintenance of physical clinics, utilities, and specialized equipment.
- Staffing Expenses: High costs associated with clinical and administrative personnel, including overtime and recruitment.
- Patient No-Shows and Cancellations: Lost revenue and inefficient use of clinician time.
- Unnecessary ER Visits: Patients seeking non-emergent care in high-cost settings.
- Geographic Barriers: The need for patients to travel long distances, incurring costs and time.
Telehealth directly addresses many of these areas, offering opportunities for substantial savings. Our focus on telehealth cost reduction aims to systematically dismantle these inefficiencies.
Pillars of Optimized Telehealth Workflows for Cost Reduction
Achieving a 10% cost reduction by 2026 requires a multi-faceted approach, focusing on several key areas of telehealth workflow optimization. Each pillar contributes to the overarching goal of enhanced efficiency and fiscal prudence.
1. Streamlining Patient Intake and Scheduling
The initial touchpoints of patient engagement often present significant opportunities for efficiency gains. Traditional intake processes can be time-consuming and resource-intensive. Optimized telehealth workflows leverage digital solutions to simplify and automate these steps.
- Online Patient Portals: Empower patients to complete registration forms, medical history updates, and consent forms digitally before their virtual appointment. This reduces administrative burden and improves data accuracy.
- Automated Scheduling Systems: Implement AI-powered scheduling tools that can integrate with provider availability, send automated reminders, and allow patients to easily reschedule or cancel appointments, minimizing no-shows.
- Pre-Visit Questionnaires: Digital questionnaires tailored to the reason for visit can gather essential information, allowing providers to prepare more effectively and streamline the actual consultation.
- Eligibility Verification: Automated insurance verification systems can reduce administrative time and prevent billing errors, a significant source of telehealth cost reduction.
By digitizing and automating these processes, healthcare systems can significantly reduce the administrative staff time required per patient, leading to direct salary savings and improved overall throughput.
2. Enhancing Virtual Consultation Efficiency
The core of telehealth lies in the virtual consultation itself. Optimizing this interaction can lead to better patient outcomes and more efficient use of provider time.
- Robust Telehealth Platforms: Invest in platforms that offer high-quality video and audio, secure messaging, screen sharing capabilities, and seamless integration with Electronic Health Records (EHR) systems. This reduces technical issues that can prolong appointments.
- Standardized Virtual Visit Protocols: Develop clear guidelines for providers on how to conduct virtual examinations, manage patient expectations, and document findings efficiently. Training is crucial here.
- Remote Monitoring Integration: For chronic disease management, integrating remote patient monitoring (RPM) devices allows providers to track vital signs and other metrics proactively, reducing the need for frequent, lengthy virtual or in-person visits.
- Asynchronous Communication Options: For non-urgent inquiries or follow-ups, secure messaging or e-consultations can be more efficient than real-time video calls, optimizing provider time and patient convenience.
3. Optimizing Post-Consultation Processes
The efficiency gains from telehealth extend beyond the live interaction. Post-consultation workflows are equally important for telehealth cost reduction and patient satisfaction.
- E-Prescribing and Pharmacy Integration: Direct electronic prescribing reduces errors, saves time for both patients and providers, and streamlines the medication fulfillment process.
- Digital Referrals and Coordination: Implementing digital systems for specialist referrals and inter-provider communication minimizes delays and ensures coordinated care, preventing redundant tests or appointments.
- Automated Follow-Up Reminders: Use automated systems for sending follow-up instructions, appointment reminders, and post-visit surveys, improving patient adherence and engagement without manual intervention.
- Efficient Billing and Reimbursement: Ensure that telehealth coding and billing practices are optimized, leveraging AI-powered tools to identify correct codes and reduce claim denials. This directly impacts revenue capture and administrative costs.
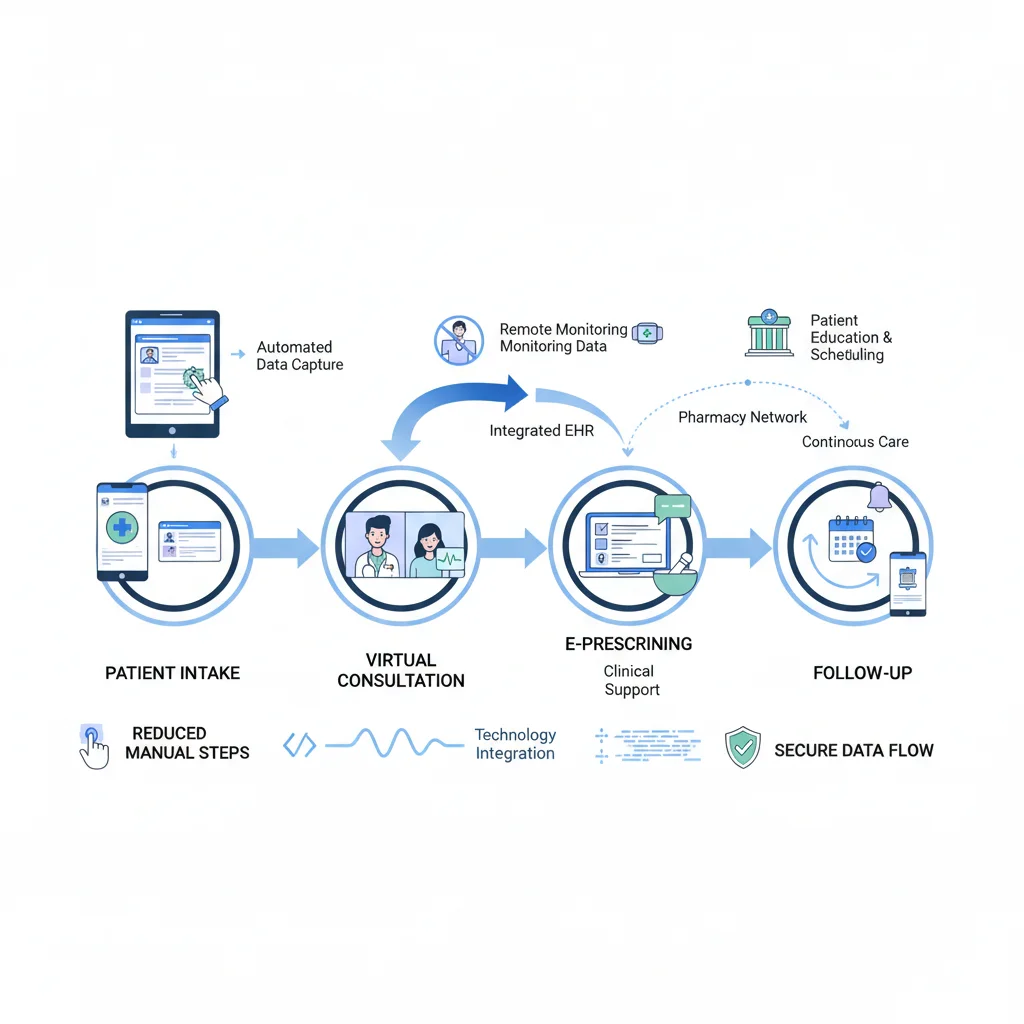
Key Technologies and Integrations for 2026
To achieve the 10% cost reduction target, US healthcare systems must embrace cutting-edge technologies and ensure seamless integration across all platforms. The future of telehealth cost reduction is deeply intertwined with technological prowess.
Artificial Intelligence (AI) and Machine Learning (ML)
- Predictive Analytics: AI can predict patient no-shows, optimize staffing levels based on demand, and identify patients at risk for readmission, allowing for proactive interventions.
- Chatbots and Virtual Assistants: AI-powered chatbots can handle routine patient inquiries, guide patients through intake processes, and provide basic health information, freeing up administrative staff.
- Clinical Decision Support: AI can assist providers during virtual consultations by analyzing patient data, suggesting diagnoses, and recommending treatment plans, improving accuracy and efficiency.
Advanced EHR Integration
The cornerstone of any efficient healthcare system is a well-integrated EHR. For telehealth, this means a platform that offers:
- Bi-directional Data Flow: Seamless exchange of patient data between the telehealth platform and the EHR, ensuring all information is up-to-date and accessible to providers.
- Single Sign-On (SSO): Simplifying access for providers to multiple systems, reducing login times and improving workflow fluidity.
- Automated Documentation: Features that allow providers to dictate notes, use templates, and leverage smart text to quickly document virtual visits, reducing administrative time.
Remote Patient Monitoring (RPM) Devices
RPM is vital for managing chronic conditions and preventing acute episodes, thereby reducing hospitalizations and emergency room visits. Wearable devices and home-based sensors can transmit data directly to the care team, enabling timely interventions and personalized care plans.
Cybersecurity and Data Privacy
As telehealth expands, so does the risk of cyber threats. Investing in robust cybersecurity measures, including end-to-end encryption, multi-factor authentication, and regular security audits, is non-negotiable. Protecting patient data is not only a legal requirement (HIPAA compliance) but also crucial for maintaining patient trust and avoiding costly breaches.
Strategic Implementation Roadmap to 10% Cost Reduction
Achieving a 10% reduction in operational costs by 2026 through optimized telehealth workflows requires a structured, strategic approach. This isn’t a one-time project but an ongoing commitment to continuous improvement.
Phase 1: Assessment and Planning (Year 1: 2024)
- Current State Analysis: Conduct a thorough audit of existing telehealth infrastructure, workflows, and associated costs. Identify bottlenecks, inefficiencies, and areas with the highest potential for telehealth cost reduction.
- Goal Setting and Benchmarking: Define specific, measurable, achievable, relevant, and time-bound (SMART) goals for cost reduction. Benchmark against industry best practices.
- Stakeholder Engagement: Involve all relevant stakeholders – clinicians, IT, administrative staff, and patients – in the planning process to foster buy-in and gather diverse perspectives.
- Technology Gap Analysis: Identify necessary technology upgrades, integrations, and new solutions required to support optimized workflows.
- Pilot Programs: Initiate small-scale pilot programs to test new workflows and technologies in a controlled environment, gathering data and feedback.
Phase 2: Implementation and Integration (Year 2: 2025)
- Technology Rollout: Deploy new telehealth platforms, EHR integrations, AI tools, and RPM devices across the organization.
- Workflow Redesign: Systematically redesign and implement optimized patient intake, virtual consultation, and post-consultation workflows based on pilot program findings.
- Training and Education: Provide comprehensive training for all staff members on new technologies and workflows. Develop educational resources for patients to encourage telehealth adoption.
- Policy and Governance: Establish clear internal policies, protocols, and governance structures for telehealth operations, ensuring compliance with regulatory requirements.
Phase 3: Optimization and Scaling (Year 3: 2026 and Beyond)
- Performance Monitoring: Continuously monitor key performance indicators (KPIs) related to cost savings, patient satisfaction, provider efficiency, and clinical outcomes.
- Feedback Loops and Iteration: Establish mechanisms for ongoing feedback from staff and patients. Use this feedback to identify areas for further refinement and continuous improvement.
- Scaling Best Practices: Expand successful pilot programs and optimized workflows across all relevant departments and service lines.
- Regulatory Adaptation: Stay abreast of evolving telehealth regulations and reimbursement policies to ensure ongoing compliance and maximize financial opportunities.
Measuring Success: KPIs for Telehealth Cost Reduction
To confirm that the 10% cost reduction target is being met, healthcare systems must meticulously track a range of key performance indicators (KPIs). These metrics provide actionable insights into the effectiveness of optimized telehealth workflows.
Financial KPIs:
- Reduction in Administrative Costs: Track staff hours spent on scheduling, billing, and patient intake before and after optimization.
- Decreased Facility Overhead: Measure savings from reduced physical space requirements, utilities, and maintenance.
- Lower Patient No-Show Rates: Calculate the financial impact of reduced missed appointments.
- Reduced ER Visits and Hospitalizations: Quantify savings from preventing unnecessary high-cost care through proactive telehealth and RPM.
- Optimized Supply Chain Costs: Indirect savings from reduced need for consumables in physical clinics.
- Improved Reimbursement Rates: Monitor the percentage of telehealth claims successfully reimbursed and the average reimbursement per visit.
Operational KPIs:
- Provider Efficiency: Measure the number of patients seen per provider per day/week via telehealth compared to in-person.
- Patient Throughput: Analyze the overall volume of patients managed through telehealth services.
- Wait Times: Track patient wait times for virtual appointments.
- Documentation Time: Measure the time providers spend on charting and administrative tasks post-telehealth visit.
- Technical Uptime and Resolution Time: Ensure the telehealth platform is reliable and technical issues are resolved swiftly.
Patient and Staff Satisfaction KPIs:
- Patient Satisfaction Scores: Gather feedback on ease of access, quality of care, and overall experience with telehealth.
- Provider Burnout Rates: Monitor staff well-being and satisfaction with telehealth workflows.
- Patient Engagement: Track adherence to treatment plans and participation in follow-up care via telehealth.
Challenges and Mitigation Strategies
While the benefits of telehealth cost reduction are clear, implementing these changes is not without challenges. Proactive strategies are essential for success.
Technological Barriers:
- Integration Complexity: Integrating new telehealth platforms with existing EHRs can be complex. Mitigation: Prioritize platforms with open APIs and strong vendor support. Invest in dedicated IT resources for integration.
- Digital Divide: Not all patients have reliable internet access or the necessary devices. Mitigation: Offer hybrid care models, provide resources or guidance on accessing technology, and ensure platforms are user-friendly for diverse demographics.
Regulatory and Reimbursement Uncertainty:
- Evolving Policies: Telehealth regulations and reimbursement policies can change. Mitigation: Stay informed through industry associations, legal counsel, and dedicated policy monitoring. Advocate for consistent, favorable policies.
Staff Adoption and Training:
- Resistance to Change: Clinicians and administrative staff may be resistant to new workflows. Mitigation: Involve staff in the planning process, provide comprehensive and ongoing training, highlight benefits, and offer incentives for adoption.
Data Security and Privacy Concerns:
- Breach Risks: The increasing volume of digital health data raises security concerns. Mitigation: Implement a robust cybersecurity framework, conduct regular risk assessments, and ensure all staff are trained on HIPAA compliance and data protection protocols.
The Future of Healthcare: A 2026 Vision
By 2026, US healthcare systems that have successfully optimized their telehealth workflows will look significantly different. They will be characterized by:
- Enhanced Accessibility: Patients will have easier, more convenient access to care, regardless of geographic location or mobility.
- Improved Patient Outcomes: Proactive care, timely interventions, and better management of chronic conditions will lead to healthier populations.
- Sustainable Financial Models: A 10% telehealth cost reduction will free up resources that can be reinvested into advanced care, research, or expanding services.
- Empowered Workforce: Clinicians will spend less time on administrative tasks and more time on patient care, leading to higher job satisfaction.
- Data-Driven Decisions: Robust data analytics will inform operational improvements and strategic planning.
The journey to achieve a 10% reduction in operational costs by 2026 through optimized telehealth workflows is challenging but undeniably rewarding. It requires a clear vision, strategic investment in technology, a commitment to continuous improvement, and the active engagement of all stakeholders. For US healthcare systems, embracing this transformation is not just about financial solvency; it’s about building a more resilient, accessible, and patient-centric healthcare future.
The time to act is now. By meticulously planning and executing these strategies, healthcare leaders can position their organizations at the forefront of digital health innovation, ensuring both fiscal health and superior patient care for years to come.